Case Description
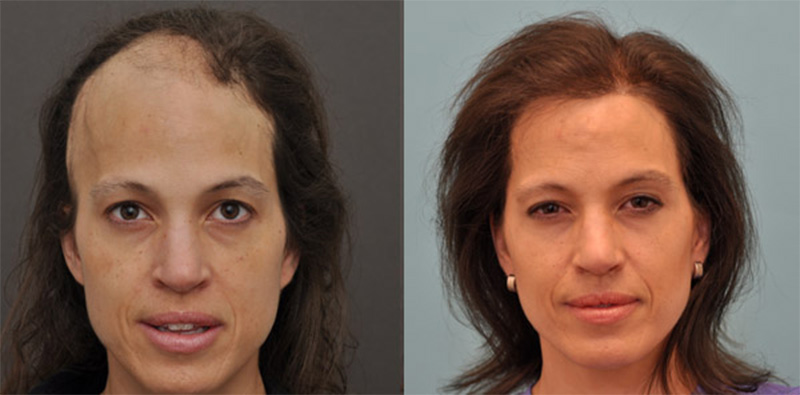
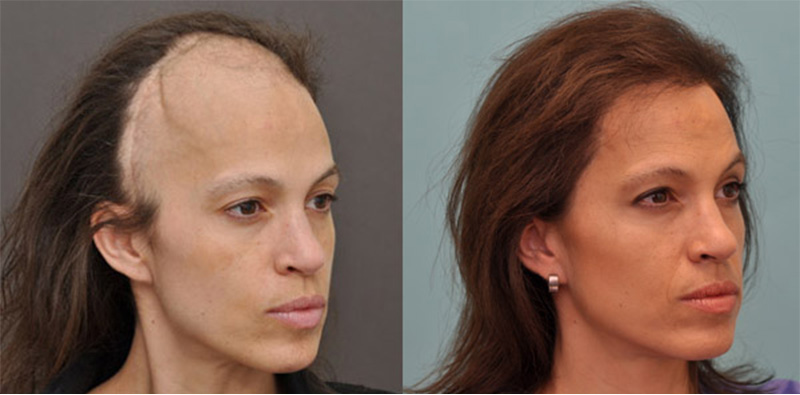
Patient History: This 40-year-old white female underwent a surgical procedure for the removal of a malignant brain tumor from the right frontal lobe of her brain and also underwent radiation therapy to the area, which led to the complete loss of her hair in that region. She was left with a cosmetically poor appearance to the entire frontal region of her scalp. She did, however, have excellent donor hair and was a good candidate for hair transplant surgery to the affected region. This case shows the capacity under the right circumstances to have a successful transplant performed on a post-radiation region of the scalp, which is sometimes considered to be situation that many surgeons would not undertake.
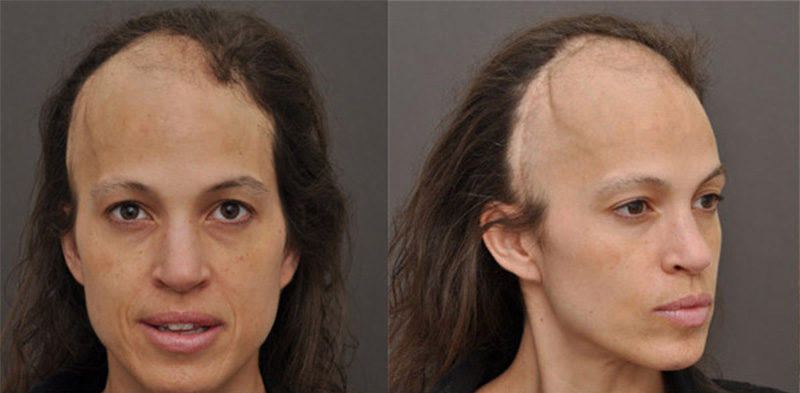
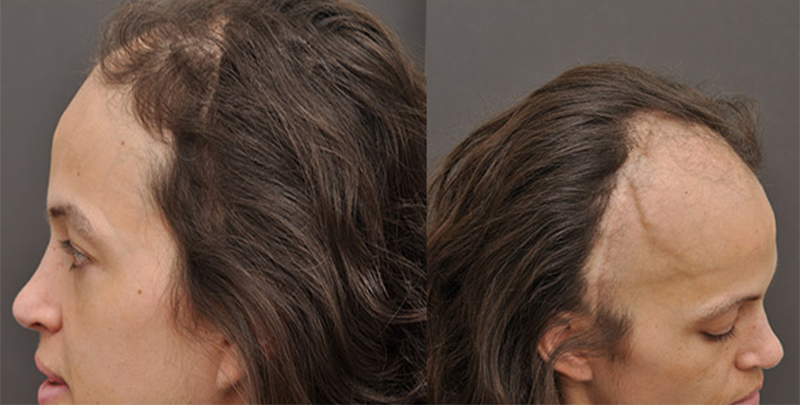
Physical Exam: The patient is a healthy white female who aside from her history of a malignant brain tumor is otherwise healthy in all respects. She was given clearance by her oncologist as being cancer free and thereby safe to proceed with a procedure.
Her hair loss extended throughout the entire right frontal/parietal region and to some extent along the left frontal region as well. Her hair texture and quality in the donor region was dark brown, very thick, and above average density at > 200 hairs/cm2.
The Plan: The patient was counseled ahead of time that she would need 2 surgeries to achieve optimal results. She understood the potential that some of the hair might not take due to her scalp having undergone radiation therapy. She did, however, have very good blood supply to the area in question, and the entire area that was to receive hair had excellent capillary refill (a simple way to test for adequate blood flow to skin tissue) The proposed procedure was to move the maximum number of grafts in the first procedure and then follow up with a second procedure at about ten months after the first procedure. The goal was to produce a natural hairline with enough density behind the hairline to allow the patient to have better hairstyling options and not to have to rely on wigs or hats to cover her scarred scalp. The challenge in this case was to transplant the maximum number of grafts possible without compromising the existing scalp and avoiding any possibility of scalp damage or necrosis.
A natural uniform hairline was imperative and achieving maximum density to the entire region was also a primary goal.
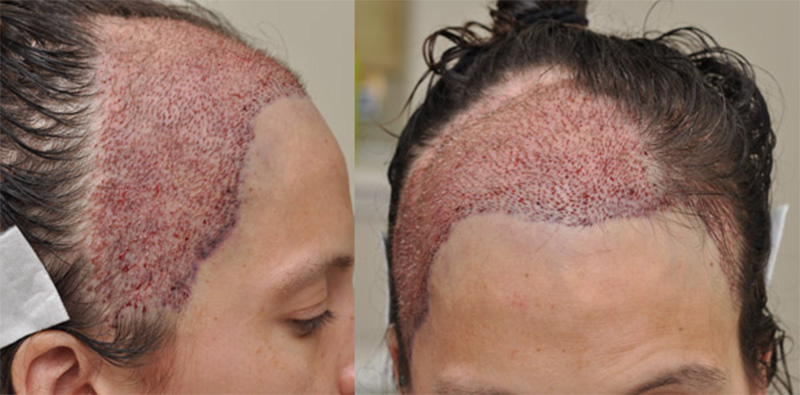
The Procedure: The patient underwent two separate transplant procedures and had a total of 4,752 grafts transplanted equaling approximately 9,000 to 10,000 hairs. We used 800 single-haired grafts to create a soft hairline and the remaining grafts varied in size from 2 to 4 hairs, distributed behind the hairline to create density. Both procedures were performed using the strip harvest method to maximize the number of hairs obtainable.
The patient had little to no scarring in the donor region and at no time throughout the process did she experience any pain or complications.


Discussion: This case demonstrated the ability to transplant into an area of the scalp previously treated with radiation but, more importantly, the ability to create adequate density combined with a cosmetically appealing hairline. The process has left our patient with the ability to style her hair and to go out in public with the confidence she desires. This case in my opinion was a complete success and despite the challenges of a large surface area and a scalp that was compromised from radiation therapy the outcome exceeded our expectations.
Return to OverviewRelated Cases
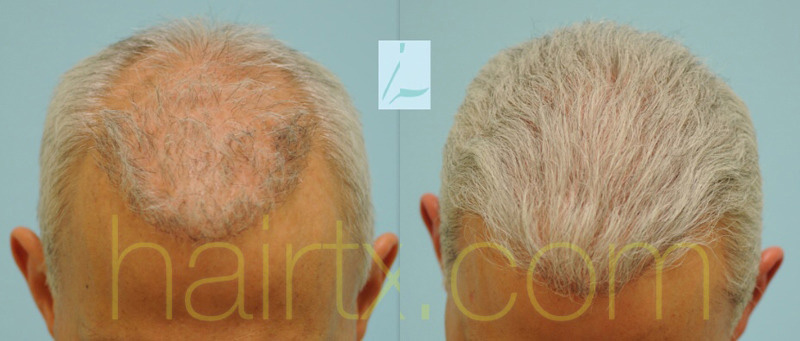
Plug & Slot Deformity Correction with Strip Harvest & Beard FUE Hair Transplant
August 24, 2022 Certified Case
Case Description History: This 54-year-old otherwise healthy Caucasian male had 5 prior hair transplants to his scalp as well as 3 scalp reductions in his…
View Case Study
FUE Hair Transplantation- Scar Tissue Following MRSA Infection
August 24, 2022 Certified Case
Case Description History: This is a 31 year old male with a history of hospital acquired MRSA infection to his scalp following colorectal surgery in…
View Case Study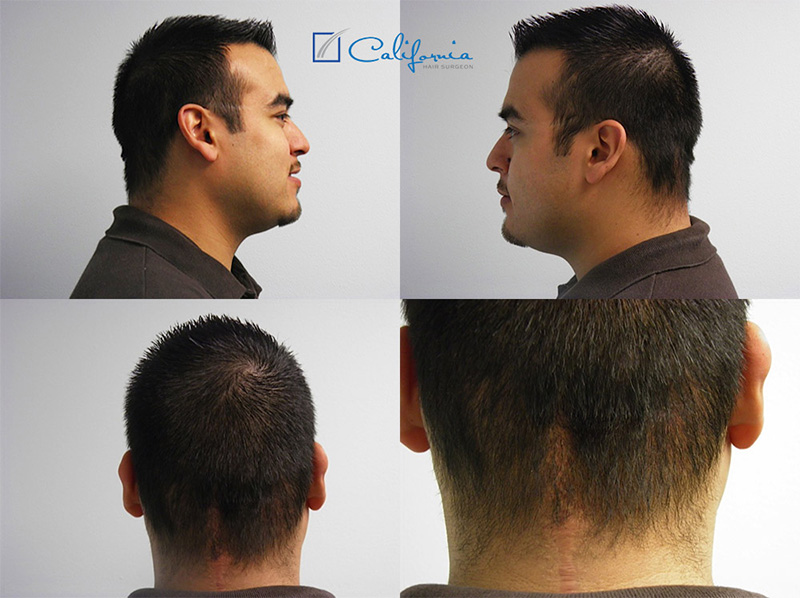
Hair Transplant Repair Of Scarring From Cancer Treatments
August 24, 2022 Certified Case
Case Description History: This 26-year-old male had a rare brain tumor known as a ganglioglioma at the age of 18. When other men his age were worried…
View Case Study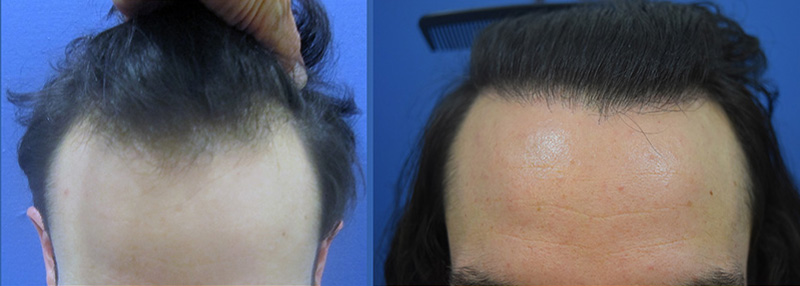
Conservative Hairline Recreation in a Young Adult Male
August 24, 2022 Certified Case
Case Description History: This 23-year-old male presents with complaints of hair loss involving the frontal hairline. He has become particularly concerned about the recession that…
View Case Study
Hair Restoration with Strip Harvest in a Male Patient with Severe Hair Loss
August 24, 2022 Certified Case
Case Description History: This is a 60-year-old healthy Caucasian male with a long history of hair loss. He stated he has a strong family history…
View Case Study